Trending
|
MPennington
A Robust and Rapid Testing Infrastructure is Needed to Identify COVID cases
Could pooled testing help resolve the backlog in testing in the US?
COVID-19 continues to rage around the United States. At the time of this writing, the US has reported over 5.46 million cases and over 170,000 deaths, more than any other country. The US has performed approximately 700 million tests, recently averaging approximately 733,000 per day. Though encouraging, this falls short of the 1.6 million daily nationwide testing target, and a recent Harvard report suggested that upwards of 20 million daily tests are actually needed. There are reports that some tests are taking over 10 days to return results. This effectively negates the utility of the test as many asymptomatic or mildly symptomatic patients may not quarantine while awaiting results, and go on to perhaps infect others. It is also estimated that there likely have been ten times as many COVID cases as identified by tests!
A robust and rapid testing infrastructure is needed as we work to reopen the economy. Testing allows us to identify infected people, isolate them, and trace their contacts to contain the spread. Until we have effective vaccines and therapeutics, testing is the best and only method we have to control the spread.
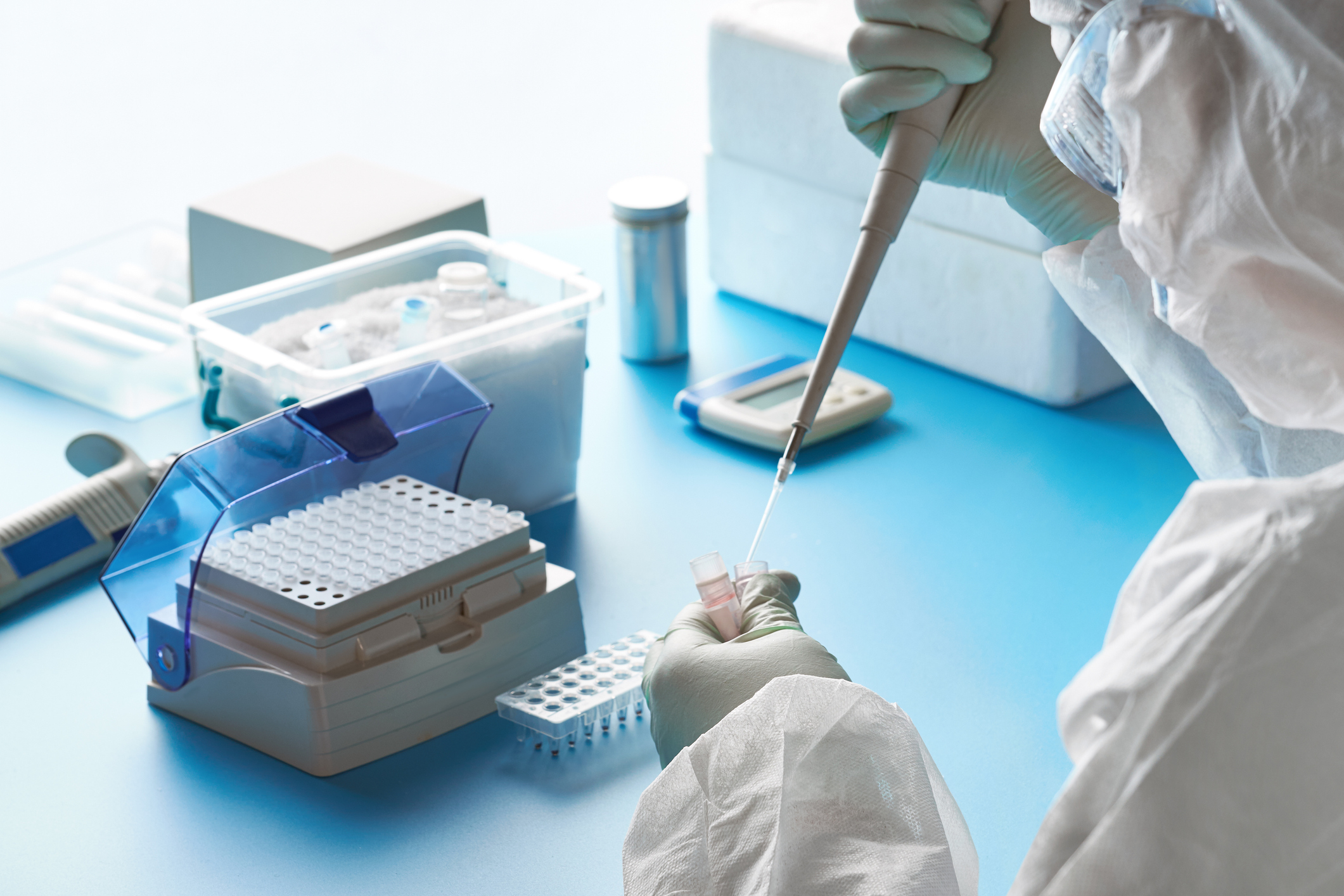
Currently molecular tests, which detect the genetic material of the virus, are most common, but require many steps to generate a result. First, a person must go to a testing location. A trained health care worker wearing proper personal protective equipment must then use a specialized swab to collect a nasal sample. The sample must be properly stored and transported to a processing lab. There, RNA is extracted and the polymerase chain reaction (PCR) is used to amplify the viral RNA. If the virus is present, amplification occurs and there is a positive signal. If there is no virus, there is no amplification and no signal. Finally, the results must be reported back to the individual.
A breakdown in any one of these steps leads to a backlog in the entire testing infrastructure. In the early stages of the pandemic, the availability of both personal protective equipment and testing locations were major limitations. Very few functional tests kits were initially available, and those that were could only be processed at the US Centers for Disease Control and Prevention, and were reserved for specific populations. The US Food and Drug Administration (FDA) quickly granted emergency use authorization for dozens of tests, allowing commercial and academic labs to process samples.
However, more issues were encountered. There were not enough nasal swabs to collect samples and there continues to be an ongoing shortage of the chemicals needed to perform the PCR reactions, leading to the prioritization of high-risk individuals over those seeking a routine test. Furthermore, the chemicals for one test are typically not compatible with another company’s test or PCR machine. These machines can only process a limited number of samples at one time, take a few hours to perform the reaction, and require skilled technicians to operate. All of these issues create bottlenecks that limit the processing of tests, leading to the delays.
Pooling Samples
Significant modifications to the supply chain and the deployment of resources to hot-spots, coordinated by a central agency, are needed to address many of the systemic issues in the testing program. In order to conserve the chemicals used in PCR, the FDA recently allowed the use of pooled coronavirus testing. This allows for four people’s samples to be grouped and tested together in the same tube. If the test is negative, all four people are confirmed to be negative. If the test comes up positive, the four samples in the pool are tested again individually to identify which were positive.
The efficiency of this method is directly linked to test positivity rate. The United States currently has ~8% test positivity rate. If 100 people were tested traditionally, 100 testing “slots” would be needed. With pooled testing, if these 100 samples were divided into 25 pools, about 8 of those pools (at most) of 4 samples would be expected to come up positive. Those pools would be separated and the 32 individual samples retested. This means that a maximum of 57 test slots are needed to generate 100 results, effectively doubling capacity. If the positivity rate was instead 20%, up to 20 of the 25 pools would be expected to test positive, and in total up to 105 test slots would be needed to generate 100 results. In this scenario, it would have been better to test the samples individually. On the other hand, as the case positivity rate decreases, larger pools could be formed, further increasing the efficiency of this method. (Wendover Productions produced a YouTube video explaining these numbers and the logistics of pooled COVID testing in much greater detail).
Bring testing home
PCR-based testing is always a lagging indicator of the caseload due to the delays between when a person thinks they may be infected, to receiving a test, to generating a result. Because of this, many companies are working to create inexpensive, rapid tests that could be widely distributed and even used by individuals on a daily basis to receive results in minutes. This would solve many of the problems identified above. Daily at home tests would largely eliminate the need for testing facilities, trained healthcare workers and PPE, and the PCR testing reagents and labs. A real time indicator of infection status could be generated, allowing people to self-isolate immediately. However, the rapid tests developed so far, which are based on detection of the viral proteins rather than the RNA, tend to have higher false negativity rates than PCR testing and there are concerns about the ability of people to appropriately collect their own samples for testing. Nevertheless, even an imperfect at home test could, in theory, help to identify a large percentage of the cases being missed with current testing capabilities.
On August 15th the FDA granted emergency use authorization to a new saliva based test. This eliminates the need for many of the specialized collection supplies, is built to use PCR chemicals from multiple vendors, and is a simpler test to run. This collectively brought the cost of a test to about $10 per sample. Results can be available within 3 hours and it has similar accuracy to traditional nasal testing. While this is a significant improvement in testing capability, its long term utility will depend on this accessibility. Further modifications and improvements will be needed to develop cheaper at home tests suitable for daily use.
We need a testing paradigm shift in the United States if we expect to be able to control the spread of COVID-19. In the short term a centrally coordinated testing response is needed to deploy supplies to critical areas and to coordinate the rapid and efficient processing of samples. Longer term, the development of more rapid, potentially at home, tests could allow for real-time screening of individuals. This would allow for self-isolation as soon as a positive case is identified, thereby limiting the spread of the virus to others. Such a robust testing infrastructure, combined with common sense safety steps such as mask wearing and proper hygiene, will allow us to stamp out the current outbreak and any flare ups so that we can all go back to work, school and our daily lives safely.
