Discovery
|
Eureka Staff
Honing in on the Early Field of Vaccines is Discovery’s Science Mission
How scientists learn, early on, whether a candidate has the juice to be potent—but not too potent
Vaccine development typically takes years, even decades. How then could companies deliver COVID-19 vaccines in a matter of months? Can we trust the process? These two questions have been dominating the airwaves ever since the first three candidates in the pipeline were authorized by regulators, a mere 11 months after SARS-CoV-2 emerged in China. We hope Eureka’s five-part series, The Vaccine Journey, on how vaccines are developed—from discovery through manufacturing—helps answer some of these questions and reassures readers that vaccines are generally very safe. Our second installment explains the key tests, early on, that determine a vaccine candidate’s future.
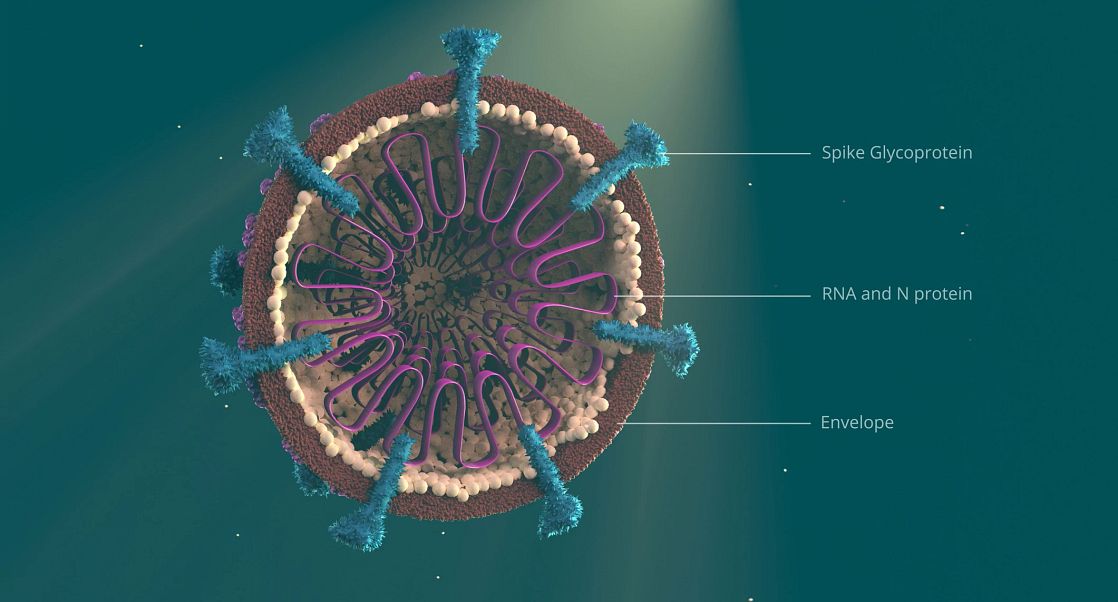
 So how do scientists go about selecting and testing the best part of the virus at driving a B cell antibody response and T cell response? They do this in large part by doing experiments called immunogenicity assays. These assays can be run in small animals and sometimes in vitro (in a dish) using blood cells donated from healthy individuals, to look at T cell responses. The assays allow different delivery systems, designs and amount of the antigen to be tested, alongside route of administration and whether an adjuvant, that helps stimulate the immune system, is required to generate an immune response. In addition, any vaccine with undesired side effects can be eliminated from the list of potential vaccines early on. For SARS-CoV-2 vaccine design, research on other coronaviruses helped inform which antigens to target and which strategies might be the most effective and which to avoid. For the reasons mentioned in Part 1 of this series, most COVID-19 vaccine research focused specifically on the spike protein of SARS-CoV-2.
So how do scientists go about selecting and testing the best part of the virus at driving a B cell antibody response and T cell response? They do this in large part by doing experiments called immunogenicity assays. These assays can be run in small animals and sometimes in vitro (in a dish) using blood cells donated from healthy individuals, to look at T cell responses. The assays allow different delivery systems, designs and amount of the antigen to be tested, alongside route of administration and whether an adjuvant, that helps stimulate the immune system, is required to generate an immune response. In addition, any vaccine with undesired side effects can be eliminated from the list of potential vaccines early on. For SARS-CoV-2 vaccine design, research on other coronaviruses helped inform which antigens to target and which strategies might be the most effective and which to avoid. For the reasons mentioned in Part 1 of this series, most COVID-19 vaccine research focused specifically on the spike protein of SARS-CoV-2.
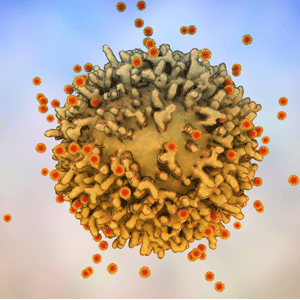
Immunogenicity assays are therefore a key determinant in a vaccine candidates’ future. As an example, suppose you were testing Candidate A, a vaccine given twice intramuscularly. If the studies failed to show antibodies were generated that could bind the spike protein, abundant T cell proliferation or release of a signature effector molecule, this would raise a red flag that the particular protein of interest, delivered a particular way failed to generate an immune response. When this occurs, developers can either reassess the route of dosing, quantity of dosing or time between injections, as well as the components of the candidate vaccine and then test again.
example, suppose you were testing Candidate A, a vaccine given twice intramuscularly. If the studies failed to show antibodies were generated that could bind the spike protein, abundant T cell proliferation or release of a signature effector molecule, this would raise a red flag that the particular protein of interest, delivered a particular way failed to generate an immune response. When this occurs, developers can either reassess the route of dosing, quantity of dosing or time between injections, as well as the components of the candidate vaccine and then test again.
It is not unusual for these studies to be redone and refined, but it takes more time and money. By assessing lots of vaccine candidates and conditions back to back, instead of sequentially and accepting that many could fail, you increase your chances of finding a promising candidate and the correct conditions for administration in a shorter time frame, without compromising on quality or safety. Fortunately for the COVID-19 candidates leading the way, the findings from the immunogenicity studies were promising, in some cases highly promising. This was mostly likely due to the fact the platforms used to create these vaccines had been studied for years, in some cases decades.
Viral vectors and RNA vaccines
Consider the viral vector vaccine now being distributed on an emergency use basis. Viral vectors are modified viruses used to shuttle genetic code for the viral antigen—in the case of COVID-19 the spike protein. The viral vector used for the COVID-19 vaccine is a non-replicating virus, it simply acts to deliver the spike antigen code into your cells but it cannot replicate, This strategy had already been extensively studied in other unrelated vaccine programs and so companies had a good idea of how much and what kind of the viral vector to use and the best way to administer it. All developers had to do was swap in the relevant COVID-19 antigens .
Extensive work had also been done on messenger RNA (mRNA) vaccines over the years. mRNA vaccines encoding the spike antigen instruct the body to make spike proteins of SARS-CoV-2. Our immune system is then stimulated to make antibodies to block the virus as if you were infected and build your B cell and T cell immunity against the virus in the future. It takes much less time to make messenger RNA than the protein antigens, making mRNA vaccines a much quicker process than traditional vaccines.
With mRNA there is also no integration into the host genome. It’s a very transient expression, meaning that the lifetime of the RNA itself will be relatively short. This also holds true for the viral vector candidate as the vector is non-replicating. This should be reassuring for people worried about the design of these novel vaccines.
The efficacy model
 Once the part of the virus or antigen that drives an appropriate immune response and the vaccine format for delivering it has been selected, the ability of the vaccine to protect from infection in an appropriate animal model, known as an efficacy model, is tested. Animal models are chosen based upon whether they can be infected by the virus and display similar features and clinical signs of disease as observed in humans. This step is important as it tells us not only is an immune response generated but whether it protects against infection and associated clinical signs and pathology. These efficacy experiments can also help identify any vaccine candidates that may stimulate the immune response in an incorrect manner and again these vaccines can be removed from the pipeline.
Once the part of the virus or antigen that drives an appropriate immune response and the vaccine format for delivering it has been selected, the ability of the vaccine to protect from infection in an appropriate animal model, known as an efficacy model, is tested. Animal models are chosen based upon whether they can be infected by the virus and display similar features and clinical signs of disease as observed in humans. This step is important as it tells us not only is an immune response generated but whether it protects against infection and associated clinical signs and pathology. These efficacy experiments can also help identify any vaccine candidates that may stimulate the immune response in an incorrect manner and again these vaccines can be removed from the pipeline.
Of course, we won’t know yet what the quality and duration of the COVID-19 vaccine-driven immune responses will be over time. The initial efficacy of the vaccines in circulation are very promising, but it is possible we may see waning immunity at some point and boosters may be required.
Another unknown is the effect of COVID-19 mutations. Although this virus has a lower mutation rate than influenza, for example, there is still the potential for it to mutate to evade the immune response . Having vaccine formats that could be easily adjusted to reflect the dominant viral strain could be an advantage in the future. What is clear is that we must keep studying this and other emerging viruses and pathogens to make sure that we are fully equipped to react rapidly and safely to future pandemics.