What are Macrophage Cells?
A macrophage cell’s primary role is patrolling for potential pathogens, then destroying the pathogen by engulfing it. Because human macrophages possess the ability to eliminate pathogens and recruit and instruct other immune cells, they play a central role in protecting the body and contribute to the pathogenesis of inflammatory and degenerative diseases. Macrophage cells can modify themselves and change their functional phenotype depending on the presence of environmental cues.
Human macrophage cells are derived from purified CD14+ monocytes. CD14+ monocytes are positively selected via immunomagnetic beads and are cultured for several days in the presence of stimulating factors to promote differentiation. Human macrophage cells possess functional plasticity and are generally classified into two main categories, M1 and M2, based on activation and function. Macrophage cell phenotyping is confirmed by morphology and the expression of specific biomarkers.
High-Quality Macrophage Cells for High-Quality Results
Charles River macrophage cells are guaranteed to have >90% purity and >80% viability as measured by flow cytometry.
Human macrophages are differentiated from freshly isolated CD14+ monocytes and are then cryopreserved in a serum-free and protein-free fully defined cGMP CryoStor™ CS10 cryopreservation medium (BioLife Solution, Seattle, WA).
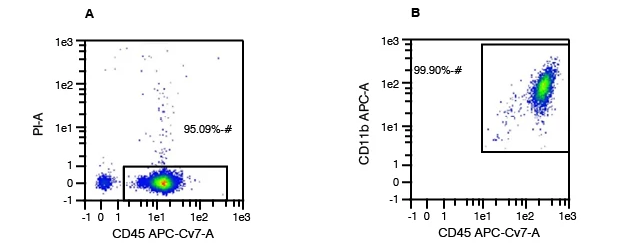
Figure 1. In Panel A, CD45 and Propidium Iodide (PI) are used to assess purity and viability of PBMCs. CD45 is expressed on all leukocytes and is used to indicate purity of the white blood cell (WBC) component. Because PI cannot pass through the membrane of live cells to stain DNA, it serves as an indicator of viability. Representative data shown here indicates purity of 95.09%, meaning >95% of cells in this sample are WBCs. (May not be indicative of received samples.) In Panel B, CD11b is the surface protein involved in adhesion between several different cell types and is expressed on the surface of monocytes, macrophages, and granulocytes. When comparing levels of CD11b versus expression of CD45, the purity of the sample for macrophages can be assessed. This graph shows a representative data set with purity of 99.90% after differentiation in culture. (Actual purity may vary from sample to sample.)
Which Human Macrophage Product is Best for your Research?
Macrophage cells are generally classified into either M1 or M2-type cells based on the environmental conditions under which they become activated, and their subsequent phenotypic expression and functional role as part of the immune response. Customers may purchase M1, M2, or mixed human macrophage cell populations depending on their research needs.
- M1 macrophages - M1 type, or classically activated macrophages, produce pro-inflammatory cytokines, mediate resistance to pathogens, and exhibit strong microbicidal properties. M1 macrophage cells are derived from purified CD14+ monocytes. CD14+ monocytes are positively selected via immunomagnetic beads and cultured in the presence of GM-CSF for 10 days. The M1 phenotyping is confirmed by morphology and the expression of specific biomarkers.
- M2 macrophages - M2 type, or alternatively activated human macrophages, play a central role in response t o parasites, tissue remodeling, angiogenesis, and allergic diseases. M2 macrophage cells are derived from purified CD14+ monocytes. CD14+ monocytes are positively selected via immunomagnetic beads and cultured in the presence of M-CSF for 10 days. The M2 phenotyping is confirmed by morphology and the expression of specific biomarkers monitored by flow cytometry.
- Mixed Macrophages - Mixed macrophage cell populations are derived from purified CD14+ monocytes. CD14+ monocytes are positively selected via immunomagnetic beads and cultured in the presence of GM-CSF or M-CSF for 10 days. Along with M1 and M2 macrophages, more rarely expressed macrophage subpopulations may also be present.
M1-type and M2-type macrophage cells from Charles River may be purchased separately or as a mixed product. Freshly isolated macrophages should be used immediately upon receipt. If not used immediately, temporarily store cells at 0-4°C or freeze for long-term storage. For cryopreserved macrophages, either prepare cells for long-term storage in Liquid Nitrogen vapor phase or thaw for use. Storage in liquid phase nitrogen is NOT recommended. Short-term storage of cells (less than 2 weeks) at -80°C is acceptable but should be minimized to ensure maximum stability. Once thawed, samples must be used immediately.
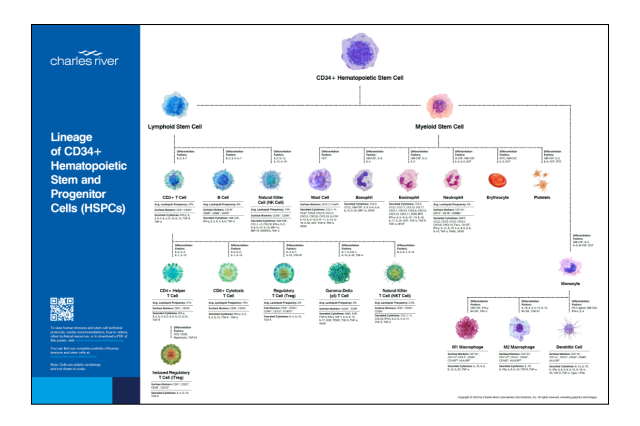
Lineage of CD34+ Hematopoietic Stem and Progenitor Cells (HSPCs)
Receive a complimentary poster to access information on immune cell markers, differentiation factors, cytokines, technical protocols, media recommendations, how-to videos, and more.
Human Macrophages in Cell Therapy
Macrophage-based cell therapy approaches are being studied for their efficacy in treating many different serious and life-threatening conditions, including cancer, spinal cord injury, and autoimmune disease. Several of the more noteworthy applications are described below:
-
Cancer immunotherapy
CAR-T cell therapy has met with unprecedented success for treating blood-based cancers but not solid tumors. Pro-inflammatory macrophage cell subtypes are capable of infiltrating the tumor microenvironment and are being investigated for their capacity to fight solid tumors.
-
Tissue injury
Human macrophage cells play a key role in skeletal muscle regeneration after injury. Multiple clinical studies are investigating the therapeutic potential of macrophages for treating acute tissue injury, including speeding wound healing, and limiting post-injury tissue inflammation and degradation following spinal cord injury.
-
Autoimmune disease
Monocytes and macrophage cells play an important role in regulating the immune response and are involved in the initiation, development, and resolution of many inflammatory disorders. The presence of activated macrophage cells is a hallmark of several autoimmune diseases, and recent evidence suggests that inappropriate macrophage activation may be at least partially responsible for the initiation of such disease. A better understanding of macrophage activations mechanisms could lead to better therapeutic treatments for autoimmune diseases.